When should MRIs be ordered?
- claytonchiropractic
- 2 hours ago
- 6 min read

The majority of people listening to my podcast will not be able to order advanced imaging of patients. Most of my listeners are attorneys and unable to order MRIs, but I wanted to take some time today and discuss indications for advanced imaging. I have worked with some attorney’s I am sure none that are listening to this podcast, but ones who demand MRIs on every case. This is dishonest and should not be done. We need a clinical justification for ordering advanced imaging.
Today’ study is Role of Magnetic resonance imaging in acute spinal trauma: a pictorial review: published in the BMC musculoskeletal disorders journal in 2016 by Yogesh Kumar and Daichi Hayashi. Their study showed that x-rays and CT scans are the initial imaging in the diagnosis of most cases of spinal injuries. A CT scan is basically an x-ray machine capable of taking multiple x-rays in a matter of seconds and compiling all them into a picture. CT is best to see fractures and bleeding. Almost without failure if advanced imaging is required for diagnosis in the emergency room CTs will be done. This is due to the fact that fractures, instability and bleeding are serious potentially life-threatening injuries.
They reported that MRIs are the modality of choice for evaluation of the ligamentous and other soft tissue structures like disc and spinal cord. The MRI is also useful in diagnosing occult or difficult to see boney injuries. Most of the soft tissue injuries seen on MRI are less life threatening and are not always emergent. Of course, spinal cord compression would be an emergency need for an MRI.
This study has 6 indications for ordering an MRI of the spine in emergency settings:
1. X-rays or CT scans show signs of ligamentous injury.
2. To look for an epidural hematoma or disc herniation before attempting a closed reduction of cervical facet dislocations.
3. To identify spinal cord abnormalities in patients with suspected spinal cord damage.
4. To exclude clinically suspected ligamentous or occult bony injuries in patient’s with negative x-rays or CT scans.
5. To assess stability of the cervical spine and need for cervical collar in patients who have altered mental status.
6. To differentiate between bleeding or nonbleeding spinal cord injuries.
This study went on to show the following benefits from MRIs over CT scans:
Higher sensitivity for detection of ligament injuries, able to diagnose disc damage and herniations, Able to detect more vascular injuries, able to detect spinal cord injuries, can help distinguish new vs. old fractures, Can help evaluate benign vs malignant fractures.
When indicated they recommend getting an MRI within 72 hours of the injury to assess for the hyperintensity of the T2 to edema making ligament and bleeding injuries more visible. Unless imaging is ordered in the emergency room it will be difficult to see MRIs within 72 hours most of the time. This means that we may be missing some or all of the edema in ligaments and muscles after an injury.
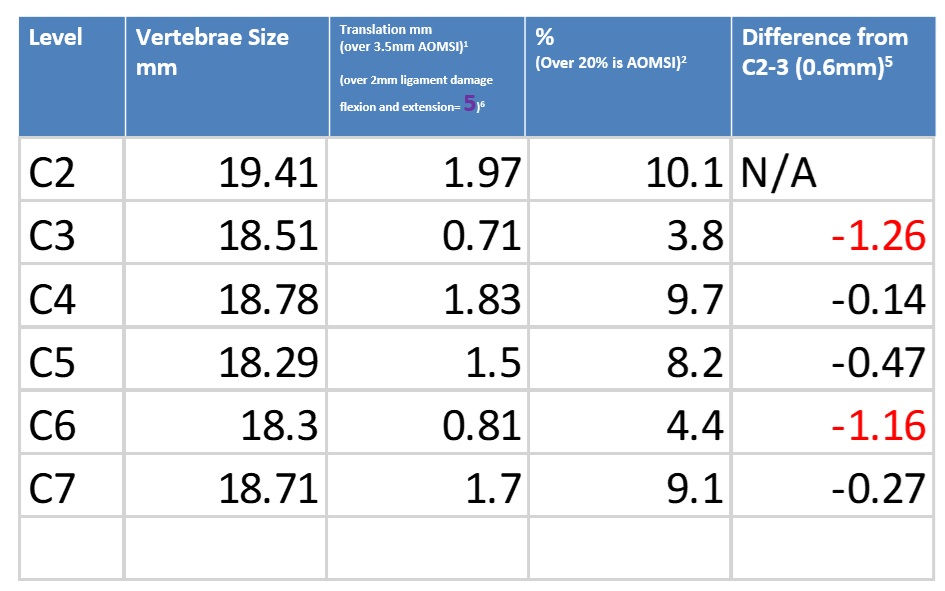
We have talked in past podcasts about how we use x-rays to assess for ligament damage in the spine. We can take measurements with flexion and extension x-rays and assess the damage to ligaments. If we have the MRI shortly after an injury, we can see signs of ligament damage as well. New ligament damage will have an increased signal on a STIR view.
MRIs are helpful at assessing disc damage. A new herniation is a disc that has nucleus pulposis herniating out of the annular fibrosus. This study showed that traumatic or new disc herniations are often associated with vertebral fractures, dislocations and hyperextension injuries. This study showed that MRI is better at showing contrast between disc, bones and csf. MRI is best at showing possible disc fragments and nerve abutment or compression.
This study showed that discs can be damaged without herniation. This is seen with widening or narrowing of the disc with abnormal signal related to edema.
Although CT is the gold standard for fractures MRI is very useful. They reported that compression and cortical breaks are hard to diagnose with CT and MRI is very sensitivity for showing these occult osseous injuries. The MRI will show marrow edema (or modic changes) as we have talked about in the past. This study went on to show that compression fractures of vertebra are very common. If a compression fracture is seen on x-ray or CT it can be difficult to assess if this is a new or old fracture.
New fractures will have bleeding and edema which increase the fluid content in the bone and this can be seen on MRI. We have covered this in past podcasts and is a type 1 modic change. Chronic fractures will not have the bleeding or edema and will not show type 1 modic changes. Often old fractures will have marrow replaced by fat tissue and this can also be seen on MRI. Fatty marrow changes will be seen as a type 2 modic change. Really old sclerotic fractures can also been seen on MRI as type 3 modic changes. This study makes an argument that MRIs should be used to help differentiate a new vs. old fracture.
This study showed that there are pitfalls of MRIs. The first problem is the artifacts given off due to metallic hardware. This can make MRI difficult to see anything. There are different MRI sequences that can help with artifacts, but it is not perfect. MRIs take a lot longer than a CT scan. A CT scan can take just a couple seconds, but an MRI can take 20-30 minutes an area. The longer the study the more difficult it can be for the patient to hold still. Movement during an MRI can create a motion artifact and this will decrease the quality of the study.
When we have motion we can not control during an MRI like the flow of blood. This is often compensated for with saturation pulses. These saturation pulses can increase the quality of the MRI, but also can mask other findings.
This study shows one of the most common mistakes I came across in my MRI training with the neuroradiologist. Lots of patient’s have prominent epidural veins. These epidural veins have a high signal of STIR and T2 images and can be confused with a disc herniation or edema. This study reported that veins appear as well-defined linear areas of high signal. With experience and training it becomes easier to distinguish between pathology and epidural veins. When I was in New York doing the mini-fellow ship with the neuroradiologist we covered a few cases just like this. This is most commonly seen in the cervical spine from my experience.
There are times that you can’t be sure if there is a small disc herniation or just prominent epidural veins. I have written in reports that there is a likely prominent epidural vein, but that a small disc herniation can’t be ruled out.
This study concluded following spine trauma a CT is adequate to determine stable vs. unstable. They also concluded that MRI can offer additional help with ligament damage, bleeding, and spinal cord injuries.
Real world example
In my training I have been taught to order an MRI for a patient on the initial examination if there is suspicion of nerve involvement. If there is signs and symptoms of nerve root or spinal cord pathology. Given the lack of neurological involvement we typically do not order MRIs on the first visit. If the patient gets worse or is not showing the progress expected then advanced imaging should be considered in the next month. Today’s study is a good refresher on other times we may consider ordering an MRI when there are no apparent signs and symptoms of nerve involvement.
I had a patient that was in a MVC and came in for care. He was rear-ended by a large truck pulling a trailer on the freeway. This collision would have created a massive amount of force capable of causing serious injuries. X-rays were taken in my office to assess for stable vs. unstable injuries. There were endplate disruptions in his thoracic spine from T6-12 or indentations in the top of the vertebral bodies. The patient had the genetic condition Klinefelter syndrome. Klinefelter’s syndrome adversely affects testicular growth which leads to less testosterone. This lack of testosterone can lead to weak bones. Given the potential for weaker bones and x-rays showing endplate disruption is raised the suspicion of new fractures in the MVC or old fractures from a life of weaker bones.
Given the lack of neurological symptoms on the examination an MRI would not typically be ordered. In this case I ordered an MRI to assess new vs. old fractures. This would be important to know for how to clinically manage the patient and causation for his legal case.
The MRI showed type 1 modic changes on the T7 end plate disruption. The Type 1 modic change is increased signal on a T2 and STIR showing edema and a decrease in the T1 signal. This shows that the endplate disruption at T7 was a new fracture to his vertebra. This altered the treatment plan and was able to show that he did in fact have a new fracture in his thoracic spine.
This is a good example of clinically justifying an MRI to help manage a patient’s injury without any neurological involvement on examination.



Comments