Do new herniated discs have height loss?
- claytonchiropractic
- 2 hours ago
- 6 min read

The last few podcasts have been about time dating injuries with MRI. Today’s podcast will not be specific to just MRI, but will be useful with CT and x-ray. Keep in mind that all methods for time dating injuries just help paint a picture. Will all of the evidence add up to show a new injury, or will the evidence stack up to show a pre-existing injury unrelated to recent trauma.
Today I want to go over 2 separate studies. The first study is The diagnostic value of an x-ray based scoring system for degeneration of the cervical spine: a reproducibility and validation study. This study was published in the Pain practice journal in 2021 by Maarten vaneerd et al.
This study reports that there are 5 features seen on radiographs that are features of degeneration. Remember degeneration takes months to be seen on imaging and years to develop and is not related with a new injury. The five features are disc height loss, anterior vertebral osteophytes, posterior vertebral osteophytes, vertebral end plate sclerosis and uncovertebral osteoarthritis. Or in other words disc space height loss and bony changes. We talked about Wolffs law and bony changes during our last podcast. Remember Wolff’s law states that bones will adapt to the loads under which they are placed. Once we alter the function of a joint we will change the loads on the bones and create bony changes seen on imaging 6 months to years later.
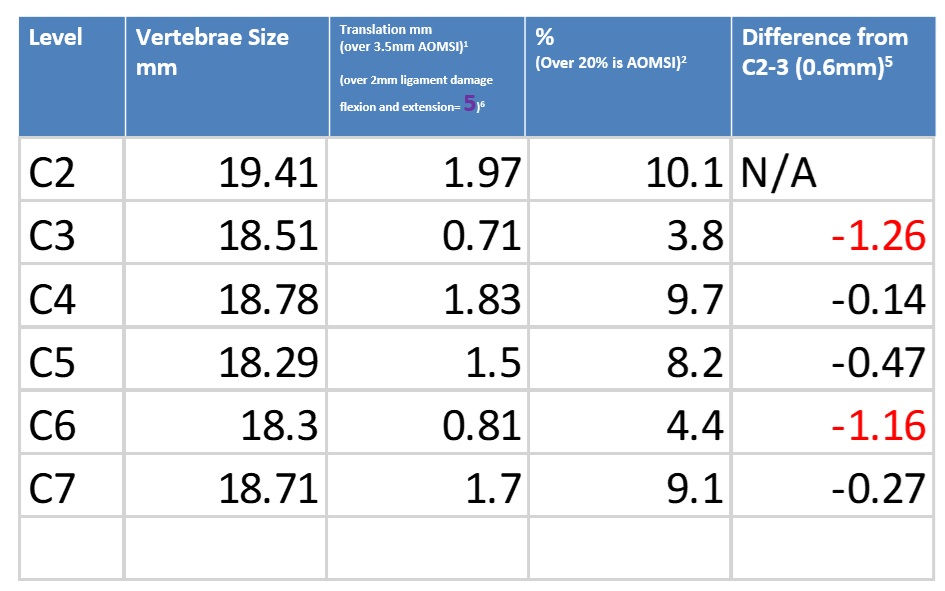
Today we will focus the podcast mostly on disc space loss. This can be seen on x-ray, CT and MRI. The MRI is best to evaluate the discs, but disc space height loss can be seen on any of the images. Disc space height was measured in the middle of the disc. What they showed was that the disc space should be ruffly 3 times smaller than the vertebra below the disc. They defined the vertebral height as measuring the posterior vertebra.
What a simple way to see if we have disc space loss. If we do have disc space loss then we have one indicator that we are dealing with a degenerative and older injury. If we have no disc space loss then we have one more indicator that we are likely dealing with a new injury.
This study did define how to assess for the bony degenerative changes. They reported that if we are looking for anterior or posterior bone spurs we should draw a line running down the lower anterior or posterior corner of C2 and the middle section of the C3-7 vertebra. If we have any bony outgrowths sticking out beyond the line then we have degenerative changes that are an indicator that there is pre-existing changes.
Endplate sclerosis is easy to see on MRI and often has a type 3 modic change, but on x-rays and CT scans the endplate sclerosis is there if we have broader or whiter and irregular endplates. If we have this sclerosis we know that the forces placed on the bone has changed and over time developed the bony changes and we are likely dealing with a pre-existing injury.
The second study I want to go over today is the role of radiography in the study of spinal disorders published by Fernando Santiago et al in the quantitative imaging and medicine and surgery journal published in 2020. This study reported that 70% of spinal pain is classified as non-specific (meaning the source can not be identified). This non-specific spinal pain was broken down into 2 categories. The first was a strain/sprain injury of the soft tissues and the second was mechanical back pain. They reported that these mechanical changes to the spine will lead over time to degenerative changes seen on imaging.
They reported that with most injuries x-rays are the initial diagnostic tool, but that often x-rays do not lead to any specific diagnosis and MRI would be the next diagnostic exam. This study reported that there are features seen on imaging that help distinguish new vs. old changes. These features are normal vertebral height and lack of bone spurs.
This second study talked about what type of imaging to order with trauma. They say CT scan or x-rays should be the initial imaging after trauma unless we have neurological compromise or ligament injury and then we should get MRIs. The use of MRI for ligament injury is not done in the spine, but more for extremities. They report that flexion and extension x-rays are done to evaluated ligament injuries in the spine. They reported that ligament damage in the spine is seen with anywhere from 1 to 3.5mm translation. This is consistent with our first podcasts about ligament damage.
This second study showed some features of an older injury are seen with osteochondrosis which is characterized by narrowing of the disc space, central vacuum phenomenon which is the collection of gas in the disc space, sclerosis or hardening of the vertebra and osteophytes or bone spurs in any direction. They went on to show that these degenerative changes showing an old injury are often asymptomatic in patients.
This second study reported that degenerative old injuries are associated with abnormalities including disc space height loss and bulging discs.
These studies have shown us ways to look at imaging and help understand a new vs old injury. Most of this information we have gone over is past podcasts, but the loss of disc space height and how to measure is new. To reiterate the loss of disc space height is a disc that is less than 1/3 the size of the vertebra below the disc.
These articles might not seem like headline news or earth shattering information, but they do help with one more part of the puzzle of time dating injuries with imaging.
Real world
I had a patient with neck pain and radicular complaints. Examination showed that she likely had radiculopathy and an MRI was ordered. The MRI showed disc damage at 3 separate levels. 2 of the levels showed a loss in disc height with bone spurs. These 2 levels showed circumferential disc bulges with neural canal stenosis, but no nerve root compression. She reported being in 2 prior MVC over the last 16 years. The MRI showed 1 level of disc herniation (or focal disc damage). As seen in today’s study, she did not have disc space loss at this level. This was shown by measuring the middle of the disc and the posterior of the vertebra. As long as the vertebra is 3 times the disc space then there is no loss of disc space. There was a focal protrusion type disc herniation with nerve root abutment, but no compression. There were very minimal bone spurs surrounding this disc herniation.
Now if I am adding all the evidence together it becomes clear that we are dealing with a patient that has findings that likely came from her prior MVCs over the last 16 years. The 2 disc bulges with disc heigh loss and bone spurs appear chronic and were not likely caused by the recent MVC. Once findings like this show up on an MRI the insurance companies often claim all findings in the cervical spine are pre-existing. Once this patient had 2 level disc damage the degenerative process will take over. This process will lead to circumferential disc bulges, bone spurs and loss of disc space height. Over time these changes will affect the function of her entire spine and can lead to bone spurs and other degenerative changes at other levels.
We are likely seeing these changes at the other levels with the mild bone spurring. The protrusion type disc herniation is much more likely than not new and caused by her recent MVC. The herniation appears new given the focal herniation and no loss of disc space height. As seen in today’s article and prior articles we have reviewed once the disc is damaged there will be over time a loss of disc space height and bone spurs. This can be objectively shown on imaging and makes a great contrast with the other 2 levels of disc bulges.
On top of this evidence, it really helps to know that there is a new onset of pain and radicular pain following a traumatic event. The degenerative changes in her spine would have made her cervical spine prone to injury with less force. This information will allow adjusters and attorneys to better understand the true value of her case.
Hopefully today’s studies help you understand how disc space height can help time date and injury with imaging. Keep in mind that this is just one part of the picture and when time dating an injury, we need to look at all options. I will continue to share ways to time date injuries with MRI over the next few podcasts.
Thanks for listening and please subscribe so you don’t miss out on more of the medical legal research.



Comments